____________________________________________________________________________________________________________________________________________
Key Takeaways
It is not just for the final days
Palliative care is a broad support system that can begin at the point of diagnosis and last for years, often running alongside curative treatments to manage symptoms and stress.
Focuses on quality of life
The primary goal is to manage physical symptoms, such as pain, breathlessness, and fatigue to maintain comfort and independence. It also provides emotional and spiritual support to help navigate challenges of serious illness.
Restores independence at home
Choosing home-based care allows patients to maintain their privacy and ‘home comforts’ in a familiar, calm environment. This approach helps avoid the distress of hospital stays and supports a more peaceful recovery.
Relieves the family burden
Specialist nurses and carers handle complex clinical tasks and medication, removing the logistical burden from the family. This allows loved ones to step back from being providers and focus on being a supportive daughter, son, or spouse.
Holistic emotional support
Beyond physical care, it provides essential emotional and spiritual support to help both the patient and their family navigate the challenges of a life-limiting illness.
____________________________________________________________________________________________________________________________________________
Palliative care is a holistic approach to managing a life-limiting or chronic illness, focusing on making the patient as comfortable as possible by addressing their physical, psychological, social, and spiritual needs. It’s a broad type of care that can begin at any point after a diagnosis and may last for years.
Palliative care vs. end-of-life care
It’s a common misconception that palliative care is the same as end-of-life care, but they are distinct. Palliative care is a wider category of support for a serious illness and can last for a long time. End-of-life care is more specific, offered to individuals who are thought to be nearing the end of life. The goal of both is to ensure comfort, but end-of-life care also focuses on practical matters like sorting out wills and wishes.
Who is palliative care for?
Palliative care is tailored for individuals who have an illness that cannot be cured, but whose symptoms and quality of life can still be managed.
This includes those with:
- Advanced cancers
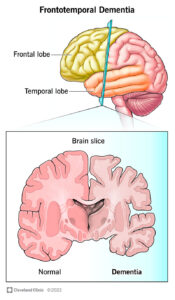
- Dementia (includng Alzheimer’s)
- Neurological conditions (such as Motor Neurone Disease or Parkinson’s)
- Advance heart, lung, or kidney disease
- Severe frailty (where multiple conditions make health unpredictable)
When does it start?
Unlike end-of-life care (which usually refers to the final 12 months), palliative care begins at the point of diagnosis.
- It can be provided for years, not just days.
- It can be given alongside curative treatments, such as chemotherapy, to help manage side effects and stress.
- It is often introduced during reablement, when a patient’s needs become too complex than standard home support can manage after a hospital stay.
Find out more about our palliative care at home services
The 5 stages of palliative care
Understanding the stages of palliative care can help you determine the right time to begin the process:
1. Creating a bespoke care plan
A clinical team works closely with the patient and their family to develop a personalised roadmap for support. This goes beyond a basic schedule. It is a live document which evolves alongside the individual’s condition.
- Person-centered goals – focus on what matters most to the person, whether that is maintaining the strength to attend a family event or managing symptoms to remain comfortably at home.
- Multidisciplinary input – often involves coordination between private nurse-led teams, GPs, and community specialists to ensure every medical and personal requirement is met.
2. Emotional and spiritual support
Palliative care acknowledges that a diagnosis affects the mind and spirit as much as the body. Ongoing support is provided to both the patient and their loved ones to navigate the emotional challenges of a lime-limiting illness.
- Holistic therapies – include talking therapies, such as counselling or complementary approaches like music and art therapy to help process complex feelings.
- Spiritual care – respects and facilitates diverse cultural or religious needs, ensuring that a person’s value and beliefs are at the heart of their daily environment.
3. Managing treatment
The primary objective is to ensure the patient lives a s comfortably, actively, and independently as possible. By proactively managing pain and complex symptoms we reduce the the risk of crisis and hospital readmission.
- Clinical excellence – expert nurses and trained carers provide symptom management, addressing issues such as breathlessness, nausea, or fatique.
- Relieving family burden – by handling clinical care and medication administration, allowing family members to focus on quality time and emotional connection.
4. Planning for now and the future
Advance care planning is vital for ensuring a person’s wishes are respected if they become unable to communicate them later. This involves clear, sensitive discussions about preferred priorities for care.
- Preferred place of care – while this stage can involve arranging inpatient care at a hospice or hospital, many prefer to remain at home.
- Specialist home support – for those wish to stay at home but require hospital-level medical support, live-in care or nurse-led interventions can be arranged. This stage encompasses the transition into end-of-life care when appropriate.
5. Supporting friends and family
The care journey extends to those closest to the patient. This final stage focuses on providing structured bereavement support to help friends and family navigate their grief.
- Ongoing compassion – support is generally available for weeks or even up to a year, depending on the specific needs of the family.
- Practical and emotional guidance – entails everything from signposting to specialist bereavement services to providing a consistent listening ear. Ensures that no one faces loss without professional guidance.
Who provides palliative care?
Many healthcare professionals, such as GPs and community nurses, provide palliative care as part of their standard duties. For more complex needs, a specialist palliative care team may be involved. These teams are composed of different healthcare professionals, including consultants, specialist nurses, and therapists, who can coordinate care for those with an incurable illness.
Symptoms addressed by palliative care
Palliative care is designed to address a wide range of distressing symptoms to improve a person’s quality of life. Some common symptoms include:
- Pain
- Nausea and vomiting
- Constipation or diarrhea
- Bowel or bladder problems
- Shortness of breath
- Coughing
- Loss of appetite and weight loss
- Depression
Getting palliative care at home
Choosing palliative care at home allows a loved one to remain in a familiar, comfortable environment, which can make the adjustment in care easier for everyone. Being at home means they don’t lose their privacy or other home comforts, which can make a significant difference to their well-being.
To access palliative care, you often need a referral from a healthcare professional currently involved in your care, such as your GP, district nurse, or another specialist. They can put you in touch with a local palliative care service.
How can Cavendish Homecare help?
At Cavendish Homecare we are experts in providing palliative homecare for clients who want to remain in their own homes. When it comes to your health and wellbeing, choosing the right homecare package is of utmost importance and navigating this process can be overwhelming. With Cavendish Homecare by your side, you’ll have the support you need to remain safely at home while enjoying elevated health and wellbeing.
If you would like to enquire about our homecare services, contact us on, 02030085210 or email us at info@cavendishhomecare.com.
 Back
Back